What is an MFM Consultation?
Dr. Keith Lescale consults patients with pregnancies progressing normally as well as patients with pregnancies that are considered high-risk. Often, primary obstetric providers (like an OBGYN or midwife) will refer their patients to a specially-trained Maternal Fetal Medicine physician (like Dr. Lescale) for their advice on the management of high risk pregnancies. Dr. Lescale tailors his consultation to the patient’s needs and the referring obstetric provider’s capabilities and requirements. Involving the referring obstetric provider at every stage is key to Dr. Lescale’s consultative approach to high-risk care. Prompt feedback is always provided via telephone or fax and referring providers are also provided a direct number in case they need to reach Dr. Lescale at any time. Some patients might only go to Dr. Lescale’s office once while others may see him every month for the duration of their pregnancy.
Communication with patient is just as important. Dr. Lescale believes that quality care is best facilitated when sufficient time is taken to gather all pertinent information. Dr. Lescale and his team will gather all relevant information for the patient’s current and future pregnancies to assure each patient is provided great care.
The ultimate goal of the MFM consultation is to make sure every patient feels empowered in their pregnancy by understanding how they or the fetus may be at risk, what options they have in regards to screening and diagnostics, and what precautions are recommended they take.

Genetics & Fetal Diagnosis
Routine Obstetric Ultrasound
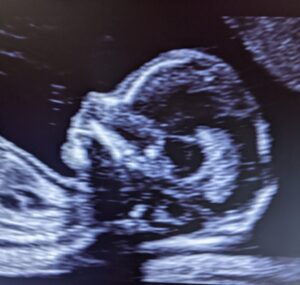
Dr. Keith Lescale offers a routine obstetrical ultrasound (sonogram). Ultrasound is very safe for pregnancy, using soundwaves to produce an image of the fetus in the uterus. Most commonly ultrasound images are in black and white, but your sonographer might use different colors (sepia, green..) to get clearer images.
Routine ultrasounds can be administered at different stages of pregnancy. In the first trimester viability and gestational age can be determined. A crown-rump measurement (length from the top of the fetus’ head to the bottom of the tail-bone) is one of the best ways to predict a patient’s due date.
An ultrasound in the second trimester usually between 18-22 weeks can be ordered to evaluate the number, placental position, and further evaluate the anatomy of the fetus.
An ultrasound in the third trimester is used to monitor the growth and positioning of the baby.
Nuchal Translucency Screening
Dr. Lescale offers early ultrasound for measurement of the fetal nuchal translucency (NT). This measurement can help predict whether a fetus may have conditions such as chromosomal differences like Down syndrome or Trisomy 18, in addition to predicting other developmental issues like heart defects. In the past, people at high-risk for these issues would simply have been offered diagnostic testing such as amniocentesis in the second trimester, which carries some risk. Early measurement of the NT allows patients to push their decision-making up a month, potentially providing earlier reassurance.
This test has been performed in the United States since 1995, but is unfortunately still not widely available. To perform the procedure the physician or sonographer needs high quality equipment and must be certified by the Fetal Medicine Foundation in London, the organization that currently set the standards and provides the software that allows the doctor to evaluate risk. Using ultrasound, the sonographer will measure the clear space at the back of the fetus’ neck. The test is painless and involves no risk to the patient or fetus. The screening must be performed between 11 and 14 weeks.
Early Genetic / 16-Week Ultrasound
An “early genetic” or 16-week ultrasound is a specialized evaluation of the fetus performed by an MFM specialist and is one of the most informative tools in the management of a high-risk pregnancy. This ultrasound is recommended for those that have a family history of a genetic disorder, have a previous child with a genetic abnormality, will be over 35 at the time of delivery, have a chronic illness, have exposure to certain medications or chemicals, or have an abnormal clinical or laboratory finding.
High resolution ultrasound is used to provide a detailed examination of the fetus and uterine contents. The exam typically includes measurements of the fetal head, abdomen, extremities, and other structures. Many aspects of the developing fetus are evaluated during this scan. The sonographer will typically get measurements of such organs as the fetal brain, heart, kidneys, bladder, and stomach, as well as many different bones like femurs, ribs, and spine. They will assess for signs of conditions like spina bifida and other neural tube defects. Fetal activity is also assessed. The sonographer records spontaneous movements of the trunk, limbs, fingers and toes, and will observe fetal swallowing and general muscle tone. Special attention is given to the appearance and movement of the heart valve, heart walls, and blood flow in the umbilical cord. The number of umbilical vessels is determined, and the volume of amniotic fluid is assessed. Finally, the placenta is measured and its size, appearance, and position described.
Level II Anatomy Ultrasound
A level II ultrasound (also known as the “anatomy scan”) is a more comprehensive or “targeted” ultrasound than a routine ultrasound. It is typically the longest of the scans during pregnancy and our team will schedule at least one hour for this ultrasound. During this scan much of the developing fetal anatomy can be visualized. Patients are referred to MFM for a level II ultrasound for such indications as:
-
- Advanced Maternal Age
-
- Multiple gestations (twins, triplets, or higher)
-
- Suspected fetal abnormalities
-
- Elevated maternal serum AFP
-
- Oligohydramnios (too little amniotic fluid)
-
- Polyhydramnios (too much amniotic fluid)
-
- Evaluation of the placenta is needed
-
- Evaluation of the umbilical cord is needed
-
- The fetus growth rate is abnormal
During the anatomy scan many birth defects can be detected. This is a good time in development to get images of certain important structures such as the brain, spine, and heart. Other structures like the fetal skeleton, gastrointestinal system, urinary tract system, and respiratory system, among others are all evaluated carefully. Fetal activity, amniotic fluid, and placenta are all assessed. However, not all problems can be visualized.
Biophysical Profile
A Biophysical Profile (BPP) is a type of non-invasive ultrasound done in the third trimester to assess whether the baby is getting enough oxygen. The BPP assigns a score for these categories: fetal body movements, fetal muscle tone, fetal breathing movements, and amniotic fluid level.
If a pregnant patient has diabetes, high blood pressure, too much or too little amniotic fluid around the baby, or is past her due date, a biophysical profile or BPP may be recommended. A BPP may also be ordered if the baby does not appear to be growing properly.
Before having the test patients are encouraged to eat because eating seems to cause good fetal movement.
Doppler Studies
Dr. Keith Lescale offers the latest in Doppler ultrasound technology. Doppler ultrasound uses sound waves to measure the flow of blood through blood vessels. MFM doppler flow studies are used to assess blood flow in the umbilical blood vein and arteries, fetal brain, and fetal heart.
This might be useful when a fetus has intrauterine growth restriction (IUGR), which means the fetus is small for their gestational age. A fetus that is not receiving enough blood, nutrients, and/or oxygen from the placenta might start to show signs of IUGR. A Doppler study can determine if the blood flow in the umbilical cord is decreased.
Recent developments in Doppler ultrasound that are available are the Power Doppler (Doppler angiography) and low energy color Doppler. Power Doppler helps to visualize the flow of blood in smaller blood vessels. Low energy color Doppler depicts the flow of blood in the fetal blood vessels in a real time scan. Different colors represent the direction of the blood flow. For example blood flowing away from the ultrasound probe looks red on the monitor, while blood flowing toward the probe is blue. Color Doppler is indispensable in the diagnosis and assessment of congenital heart abnormalities.
3D/4D Technology
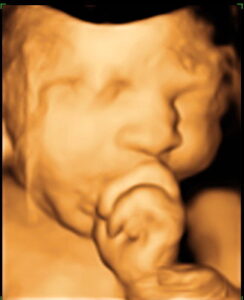
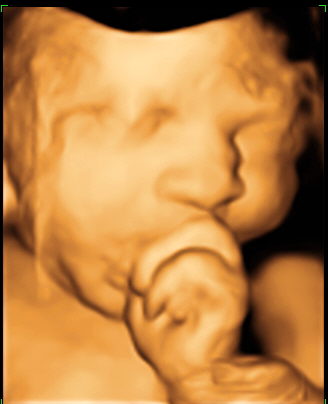
Ultrasounds are an essential tool to visualize the fetus and uterus. Traditional 2D ultrasound technology has been utilized for over 30 years and most pregnant patients have at least 2 ultrasounds during their pregnancy. Recent advances in imagery have resulted in the introduction of three and four-dimensional ultrasound, giving obstetricians who suspect a fetal abnormality a specific surface rendering of the fetus. Dr. Keith Lescale has completed thousands of scans and has been using this innovative equipment since 2002.
Physicians refer patients to Dr. Lescale for 3D/4D ultrasound to better detect fetal abnormalities and structural problems, such as cleft lip, spinal abnormalities, and cardiac deformities. According to Dr. Lescale there are a few limitations to sufficient visualization of fetal anatomy with 3D/4D technology. There will be difficulty visualizing structures or the baby’s face if there is inadequate amniotic fluid surrounding the fetus, or if the fetus has its face in the posterior position in the uterus. The 3D/4D technology is paid for by most major insurances when medically indicated.
Non-Stress Test
A non-stress test is a painless, noninvasive test used to evaluate the well being of the baby in the third trimester. The test can be ordered as early as twenty-eight weeks, and may be done as often as twice a week. Some reasons why Dr. Lescale or a referring may request a non-stress test are:
-
- Pregnancy-induced hypertension
-
- Diabetes
-
- Multiple gestations (twins, triplets, etc)
-
- Rh sensitization
-
- Unexplained elevated maternal serum alpha-fetoprotein (MSAFP) level
-
- Previous stillbirth
-
- History of premature labor
-
- Postdates (more than 41 weeks long)
-
- Intra-uterine growth restriction, IUGR (baby is growing slower than expected)
-
- Decreased fetal movement
-
- Too much or too little amniotic fluid
-
- Some cases following amniocentesis
The non-stress test monitors the fetal heartbeat and the mother’s uterine contraction. The test is conducted while the patient is lying in a chair and two elastic belts are wrapped around the belly. One belt measures the fetal heart rate and the other records any uterine contractions.
The fetal heart rate should increase as he moves. During the test if the fetal heart rate increases with more fetal movement twice in a ten-minute interval then the test is considered “reactive”. A “reactive” result means the fetus is receiving adequate oxygen at the time of the test. However, if the test is “non reactive” this may indicate the fetus is not getting enough oxygen or there are problems with the placenta. In this case the doctor will generally order more tests. It is important to remember that a “non-reactive” test does not mean something is wrong. It just means that more investigation is necessary.
Genetics and Fetal Screening/Diagnosis
Genetic Counseling
A genetic counselor (GC) is a professional with a specialized education, most often a masters degree, in genetics and counseling to provide personalized care to patients as they make decisions about their genetic health. Expecting mothers, those planning to become pregnant, and their families might expect to see a genetic counselor during their MFM consultation for many reasons. Some of these reasons include:
-
- Questions about a disease or condition that runs in the family
-
- A family history of an inherited disorder, birth defect, or intellectual disabilities or delays
-
- An abnormal result from a genetic screening or diagnostic test
-
- An abnormal ultrasound result
-
- Concerns about health, lifestyle, or work environments that might pose a risk to the pregnancy (infections, medicines, drugs, chemicals, and/or other environmental agents)
-
- A history of infertility or multiple pregnancy losses
-
- Increasing parental age (women over 35 or men over 40)
-
- Concern of being at increased risk to be a carrier of a genetic conditions due to ethnic background (some diseases are more common in certain ethnicities or ancestries)
-
- Couples that are first-cousins or other close blood relatives
How can I prepare for my genetic counseling appointment?
The GC will ask some questions about you, your family, your pregnancy history, and your medical history. Gathering this information from your partner and from your family is important. Some things the GC may ask about are:
-
- Your (and your partner’s) pregnancy history, including all current and past pregnancies
-
- Your (and your partner’s) medical and health history
-
- The health history of other members of your (and your partner’s) family, including children, siblings, and some extended family.
-
- Your (and your partner’s) ancestral background or ethnicity.
What will happen during the appointment?
Depending on the reason for the visit, there are many aspects to a genetic counseling session. You can expect the GC to:
-
- Go over your family and medical history in detail
-
- Figure out and explain your chances of having a child with a specific genetic condition
-
- Help you explore your options and make decisions about screening and testing before and during pregnancy
-
- Help you interpret test results including the accuracy and limitations
-
- Help you understand medical and genetic information
-
- Provide you with information about any abnormal results and help you understand your options
-
- Provide counseling and emotional support
-
- Refer you to support and advocacy networks
This session is intended to empower patients and their families with knowledge so they can decide if they want any genetic testing. The decision to request or refuse any genetic test is entirely up to the patient.
Non-Invasive Prenatal Screening
Non-invasive prenatal screening (NIPS/NIPT) is a method of determining whether a fetus will be born with certain genetic abnormalities as well as the genetic sex of the fetus. This screening test uses small pieces of DNA from the placenta that are circulating in the pregnant patient’s blood, called “cell-free DNA.” The test is considered non-invasive because it only requires a blood-draw from the pregnant patient and does not pose a risk to the fetus.
NIPS is most often used to look for chromosome disorders that are caused by the presence of an extra or missing copy of a chromosome (aneuploidy). Primarily, the screening looks for Down syndrome (trisomy 21, caused by an extra 21), trisomy 18 (extra chromosome 18), trisomy 13 (extra chromosome 13), and extra or missing copies of the X and Y chromosomes (the chromosomes which determine sex). The accuracy of the test varies by disorder, but can be as high as 99.9%. It is important to note that this is a screening test, and false positives are very possible.
NIPS can be done after 9 weeks gestation. Indications for this testing include advanced maternal age (women over 35, abnormal serum screening, and abnormal ultrasound results). However, this test is available to all pregnant individuals.
Chorionic Villus Sampling (CVS)
Chorionic Villus Sampling (CVS) is a diagnostic procedure performed between 10 and 14 weeks of pregnancy. The procedure involves taking a small sample of tissue from the placenta via a needle, guided by ultrasound, through the abdominal wall (transabdominal CVS) or via the vagina and cervix (trans-cervical CVS). The way the procedure is done depends on the position of the placenta, the uterus, and the fetus. Dr. Lescale specializes in transabdominal CVS.
This procedure is a diagnostic tool used to determine the genetic status of the fetus. With this test, the assessment of many genetic conditions can be done. A patient may choose to consider CVS after an abnormal screening testing like maternal serum screening or non-invasive prenatal screening, an abnormal ultrasound, advanced maternal age, a family history of a genetic condition, or by any other decision. The benefit of CVS is that results are available very early in the pregnancy and are much more comprehensive than non-invasive testing. As such, patients and their partners can make important decisions about the pregnancy. Risks and benefits of the CVS should be discussed with your doctor or with your genetic counselor.
Amniocentesis
Amniocentesis may be recommended for:
-
- Women who are pregnant or planning to become pregnant and will be 35 or older at delivery.
-
- Couples who have had a baby or a relative with a genetic condition like Down syndrome, an open neural tube defect like spina bifida, intellectual disabilities, or other birth defects.
-
- Couples who are known carriers of an inherited disorder like Cystic Fibrosis, Spinal Muscular Atrophy, Tay Sachs, etc.
-
- Couples at increased risk for a baby with an open neural tube defect or genetic condition based on pregnancy screening or ultrasound.
-
- Couples who are otherwise concerned about having a genetically atypical baby.
Amniocentesis is a diagnostic procedure that can allow for the most comprehensive genetic testing. In addition, this procedure can allow for screening for conditions like open neural tube defects and infections. This procedure can be done after 15.4 weeks of pregnancy.
Amniocentesis requires an experienced physician, usually one who specializes in maternal fetal medicine. With continuous ultrasound, the physician carefully inserts a thin needle through the abdominal wall into the uterus and withdraws a small amount of amniotic fluid.
Amniocentesis is an invasive procedure and does carry a small risk for infection, miscarriage, and preterm delivery. However, medical literature has determined that there is a not a significant increase in miscarriages in women who’ve had an amniocentesis than those who have not.
Carrier Screening
Lescale MFM offers screening for many genetic conditions that is comprehensive and accurate, and can help guide your family planning. Carrier screening is a blood or saliva test that can assess the carrier status of anyone who is pregnant or planning to become pregnant and their partners. The likelihood of being a carrier for a condition varies based on the condition and on the ancestry of each patient.
Being a carrier means that someone has one non-working copy of a gene and one working copy. Most carriers are healthy and do not have a family history of any genetic conditions. There are two ways a carrier may pass on a genetic condition to their child:
-
- Autosomal recessive inheritance – a child inherits a non-working copy from both their mother and their father
-
- X-linked inheritance – typically when a male inherits an X-chromosome with a non-working copy from their mother
There are many conditions that are inherited in these ways. Some of the most common are:
-
- Cystic Fibrosis (CF)
-
- Spinal Muscular Atrophy (SMA)
-
- Fragile X
-
- Sickle Cell Anemia
-
- Alpha and Beta Thalassemia
-
- Phenylketonuria
The American College of Obstetricians and Gynecologists (ACOG) and the American College of Medical Genetics and Genomes (ACMG) has recommended carrier screening for many of the more common disorders for all women who are pregnant or planning a pregnancy. It is possible to test for multiple conditions at once or for just a few conditions are that are higher in prevalence for an individual ancestry.